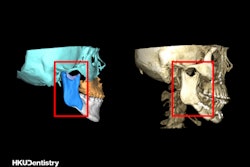
Nerve allograft surgery may be more effective and have a lower long-term cost than nonsurgical treatment for persistent trigeminal neuropathy (PTN), according to a study recently published in the Journal of Oral and Maxillofacial Surgery.
After five years, the total cost of nonsurgical treatment rises continuously and remains higher than surgical treatment. The net monetary benefits, which were calculated from a fixed willingness-to-pay threshold and which then measured the health benefits with dollars, were more than $325,000 higher for surgical treatment compared to nonsurgical management, the authors wrote.
"If surgical intervention is indicated, and the patient is interested in this option, it would be cost-effective for insurance providers to cover the costs of surgical intervention," wrote the authors, led by Dr. Benjamin Palla of the department of oral and maxillofacial surgery at the University of Illinois at Chicago (J Oral Maxillofac Surg, February 17, 2023).
According to the International Association for the Study of Pain, trigeminal nerve injuries that show no signs of improvement after three months are considered to be PTN, which affects many aspects of a patient's daily life. This condition can affect talking, eating, drinking, chewing, tooth brushing, flossing, smiling, kissing, and sleeping. Additionally, 36% of patients with trigeminal neuropathy report having depression. Other factors associated with PTN include loss of work and decreased quality of life, according to the study.
To determine which treatment was the most effective and economical, software was used to construct a Markov model that could estimate the direct and indirect costs for PTN. The model ran for 40 years with one-year cycles on a 40-year-old "model" patient who had persistent inferior alveolar or lingual nerve injury at three months post-iatrogenic nerve injury without signs of improvement and without dysesthesia or neuropathic pain. The two treatment options were nonsurgical management or nerve allograft, the authors wrote.
Using the 2022 Medicare Physician Fee Schedule, direct surgical costs were calculated. Meanwhile, nonsurgical treatment direct costs, including specialist referral, medications, and imaging, and indirect costs, like quality of life and loss of employment, were determined from historical data and research. Direct surgical costs for allograft repair were $13,291. State-specific direct costs for hypoesthesia/anesthesia were $2,127 per year and $3,168 for neuropathic pain per year. Decreased labor force participation, absenteeism, and decreased quality of life were used for state-specific indirect costs, they wrote.
The incremental cost-effectiveness ratio was -$10,751, which indicated that surgery should be used over nonsurgical management based on efficiency and cost. Over the duration of the model, the net monetary benefits of surgical treatment were $1.15 million compared to $830,654 for nonsurgical treatment, the authors wrote.
Other than the limitations of this type of model, no other shortcomings were listed.
Based on these findings, clinicians should pursue surgery for patients where this surgical intervention is indicated and a patient is willing to undergo surgery, they wrote.
"Despite high initial costs of surgical treatment with nerve allograft for PTN, surgical intervention with nerve allograft is a more cost-effective treatment option when compared to non-surgical therapy," Palla and colleagues concluded.