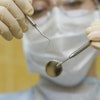
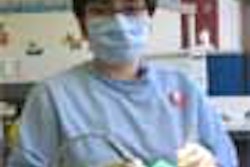
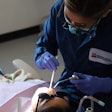
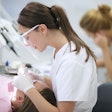
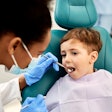
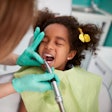
In Noorvik, Alaska where Aurora Johnson grew up, you don't have to look very hard to see the importance of dentistry. The nearest dentist is an expensive plane ride away, and many Noorvik residents can't afford the trip, much less the dentist's bill. As a consequence, "a lot of my classmates in high school graduated with little or no teeth," says Johnson.
Motivated by this first-hand experience, Johnson, 36, now wages war against caries full-time -- cajoling kids to brush their teeth, filling cavities, and when necessary, pulling teeth. But Johnson is in the midst of another war as well. She isn't a dentist -- she's a dental health aide therapist, and dentists and public health experts are battling over the legitimacy of her newly created profession. If dental therapist advocates gain momentum, they could change dental care throughout the country.
In Alaska, the battle recently pitted the American Dental Association (ADA) against the Alaska Native Tribal Health Consortium (ANTHC), a quasi-federal agency which has employed graduates of a two-year training program as dental health aide therapists since January 2005.
|
|
The ADA sued to block the therapists from performing irreversible procedures such as extractions and fillings, arguing that state law reserved that right to dentists. But a federal law gives the Community Health Aide Certification Board the power to certify the therapists. And in June, the Anchorage Superior Court ruled that this law trumps state dental licensing regulations. Rather than appealing the decision, the ADA settled, paying out $537,500 to the ANTHC. The money will go to promoting Native Alaskans' oral health in general -- and not to attorney's fees or to the dental health aide therapist program. But losing the suit bitterly disappointed the ADA leadership. "Fundamentally, we don't think dental health aide therapists are a good long-term solution to the disparities in dental care," says William Prentice, director of the Washington office. "We still think the long-term solution is to get enough dentists into under-served areas."
Since then, the ADA has tried to put the conflict behind it by focusing attention on alternative solutions for helping Alaskans and others without dental care. But now that the dental aide program has a toehold, it may be hard to stop it from spreading to other states. Already, says Valerie Davidson, senior director for intergovernmental affairs for ANTHC, she has gotten an inquiry from Arizona where an American Indian group may try starting a similar program.
Shiny smiles, deadly infections
Some public health advocates envision dental health aide therapists occupying the role that nurse practitioners or physicians' assistants now hold in the medical system. But for now, the reach of dental therapists is limited. Federal statute restricts them to working through Alaska Native organizations. Since some American Indian organizations have similar status under federal law, they might seek similar exemptions from state dental licensing regulations. No one knows what will happen if they do -- or what will happen if other remote and impoverished communities turn to Congress with requests for help.
One thing is certain: the Alaska conflict is just one symptom of a profound and festering illness in the American system of dental care. "We have the same problem in other rural places and it extends beyond the rural to inner cities where we have minorities and low income individuals," says Dennis Mitchell, D.D.S., M.P.H., who studies disparities in dental care at Columbia University. "I understand the ADA's point, and it's solid. They're concerned about creating a two-tiered system of dental care. The problem is that we already have a two-tiered system of dental care."
On one tier, people with dental insurance or plenty of money are getting whiter, shinier smiles than ever before. On the other tier, the poor and uninsured are losing teeth, suffering infections, and even dying for want of basic dental care.
The dental care problem exceeds the general crisis in healthcare, says Dr. Mitchell. "It's much larger. It's not even close." Up to 47 million people go without medical care insurance while over a 100 million don't have dental insurance. Many more have inadequate dental insurance.
The lack of dental care among the poor got national attention in June when the Washington Post reported that Deamonte Driver, a 12-year-old boy living in Maryland, died from an untreated tooth infection that spread to his brain. Driver's mother couldn't find a dentist who would accept Medicaid reimbursement, which pays less per procedure than dentists typically get. The Post reported that more than 10,780 Medicaid-eligible children in Maryland had not seen a dentist in at least four years.
And the problem of disparities are not limited to class. In October, the Journal of the American Dental Association published a study finding that Hispanic children were less likely to have dental exams, regardless of their income. Similar research has shown that African Americans, independent of wealth, are also less likely to get dental care.
Even when African Americans and Hispanics have similar access -- as they do in the Veteran's Affairs system -- they get a lower quality of dental care than whites do, says Dr. Mitchell. "Part of the reason, we believe, is that the providers don't have cultural competency," he said. "When we have a larger number of providers with the same background as the patients, the disparities are smaller."
In Alaska, problems of geography, income, and ethnicity all conspire to block access to dental care. In addition to lacking money to pay dentists, the 130,000 Alaska Natives are divided into tiny tribes in scattered villages which have different traditional languages. Some don't speak English at all. And few dentists are willing to live in a tiny Alaskan village.
As a result, Alaskan Natives experience two-and-a-half times the rate of dental caries of the U.S. populations as a whole. By recruiting dental health aide therapists from the communities they serve, the ANTHC hopes to overcome all these barriers.
"We can put dental health aide therapists in places we can't put a dentist," says Ron Nagel, D.D.S., M.P.H., one of the chief architects of the therapist program.