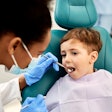
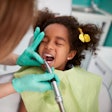
As the W.K. Kellogg Foundation begins rolling out a $16 million initiative to help five states develop midlevel providers programs similar to the dental health aide therapist (DHAT) program in Alaska, dental associations in those states remain unconvinced that this approach will be safe and effective.
While they believe directly supervised therapists can do restorations, the organizations share concerns about allowing surgical procedures such as extractions and drilling.
Kellogg's Dental Therapist Project, announced November 17, is intended to support community-based efforts in Kansas, New Mexico, Ohio, Vermont, and Washington to add therapists to dental teams providing care in underserved areas.
The goal of the three-year project is to work with local dentists, community groups, policymakers, and consumer health advocates to build consensus about improving access to care, said project director David Jordan of Community Catalyst, a national nonprofit advocacy organization that is the project's lead grantee.
"We really want to work with dentists so they're able to shape and improve access to care," Jordan told DrBicuspid.com. "This is an effort to start conversations and build the infrastructure to elevate awareness that there are significant barriers for people to get dental care."
Noting that 49 million people live in areas where there is a shortage of dental professionals and there are no dentists in many counties and rural areas, he said the project will encourage dentists to support expanded functions for dental assistants.
A recent report by the U.S. Government Accountability Office (GAO) revealed that nearly two-thirds of Medicaid children in the U.S. failed to get any dental care as recently as 2008. Some 30 million children were enrolled in the program that year.
The Kellogg initiative envisions a dental therapist who would undergo two years of technical training and then work under the general (offsite) supervision of a dentist. After getting a dentist's approval for treatments, therapists would be able to do routine extractions on mobile primary teeth and also perform restorations, including drilling, Jordan explained. Allowable extractions would not involve cutting below the gum line, he pointed out, so the procedure would not be invasive.
"They would be part of the dentist's team, and the dentist would certify their competency," he said.
Last year, Minnesota passed a law authorizing dental therapists to practice, including performing nonsurgical extractions, Jordan noted.
The dental therapist model first began in the 1920s in New Zealand and is now well-established in many developed countries, including the U.K., Australia, and the Netherlands.
In October, the Kellogg Foundation released an evaluation of Alaskan DHATs that found that these midlevel providers offer safe and competent care to residents of remote and underserved native communities.
"We're looking at an idea that has been proven and well-established," Jordan said.
Creating a two-tiered system?
But dental association officials of the five states slated for the new Kellogg program expressed concerns about allowing therapists -- who may be inadequately trained and unprepared to deal with complications that can arise even during "routine" procedures -- to perform extractions and restorations.
The Washington State Dental Association (WSDA) supports an Expanded Function Dental Auxiliary model that allows a supervised "dental extender" to place restorations but no extractions, and only after the dentist determines the diagnosis and treatment planning, according to Douglas Walsh, DDS, president of the WDA. More than 100 such workers have graduated and been licensed in Washington, and they are making a significant increase in access to care, he said.
“I think it's about turf, money, and fear.”
— Terry Batliner, DDS, Center for Native
Oral Health Research
"We wouldn't oppose anything within reason if it were under the dentist's direct supervision," Dr. Walsh told DrBicuspid.com.
Sometimes situations arise that only a dentist with adequate training and experience is competent to handle, he said. For example, many young children squirm during drilling, which could have dangerous consequences.
"Drills rotate at 400,000 RPMs, and someone who's not well-trained could have problems with something spinning that fast in a kid's mouth who is moving around," Dr. Walsh noted. "There are huge challenges."
Low reimbursement rates and cutbacks in Medicaid and other funding are the biggest barriers to access to care, he said, noting that streamlining paperwork would make handling such cases easier.
Another access issue is getting the needy into dentists' offices. "The big question is: Is it demand or need?" Dr. Walsh said. "Dentists have done a very good job dealing with demand, but need is something else." Many who need care don't know how to navigate bureaucratic programs, he said.
Dr. Walsh also wonders who will pay for a therapist's services. "Our concern is: Is it economically viable to have them?" he said.
Thomas Matanzo, DDS, president of the Ohio Dental Association, echoed this sentiment. "Who will pay for DHATs to do this treatment?" he said in an interview with DrBicuspid.com. "I don't see where the money is coming from."
Alice Warner, Kellogg Foundation program officer, noted that the new healthcare reform law mandates dental care for children, and the Children's Health Insurance Program has guaranteed funding through 2015. Also, funds are being built into new state insurance exchanges, set to begin in 2014, that will enable low-income families to buy private insurance, she said.
And a report released December 6 by the Pew Center on the States contends that private practice dentists can improve both their productivity and profitability by adding dental hygienists and dental therapists to their teams.
Dr. Matanzo is also concerned about inadequately trained staffers doing irreversible procedures without a dentist's direct supervision. The Alaska model, which involves natives in remote, tribal villages, is a unique situation, he said. "That's not like anything we have in Ohio," he noted.
Ohio has long used expanded function assistants, who can place restorations under direct supervision.
Good care involves more than drilling and extractions, Dr. Matanzo noted, such as oral cancer evaluations, diagnosing infections in the mouth and jaw, reading radiographs, and treating abscesses and trauma. "There are many other functions in which patients would be given a false sense of security that their needs are being met," he said.
He believes DHATs would create a two-tiered system that would discriminate against people in different socioeconomic or ethnic groups with a model that is "unproven" and whose cost-effectiveness remains doubtful. "This is just jumping the gun," he said.
Risk of treatment complications
Robert Manzanares, DDS, president of the New Mexico Dental Association, shares Dr. Walsh's concerns about therapists doing surgical procedures, especially if complications arise during treatment.
"What happens if you have to go deep into a cavity and accidentally go into the pulp?" he asked, adding that there is no such thing as a simple extraction or an easy filling. "What are the ramifications? If an extraction is done prematurely, there can be spacing issues, and it can cause impacted permanent teeth. Something done poorly is worse than no care," he said.
Dr. Manzanares is familiar with the challenges facing underserved communities, having grown up in an impoverished area, worked in the National Health Service Corps, and now practices in a relatively poor area.
"I see the need and how people are hurting, but we need more dentists. We need more good solutions, not quick fixes," he said. "Do we have a shortage of dentists or maldistribution? The answer to both questions is yes in New Mexico."
He supports creating more incentives for dentists, including increasing Medicaid reimbursements, noting that 43% of New Mexico dentists take Medicaid patients. He also advocates creating community dental health coordinators -- a solution being investigated by the ADA -- who would go into schools and retirement homes and help people with transportation, language, and cultural issues.
Another possibility is a collaborative dental hygienist who could use teledentistry to communicate with a dentist and assess the patient, he said, which would allow dentists to be more efficient when the patient arrives for treatment.
Dr. Manzanares also supports having an expanded function dental auxiliary who would place restorations after the dentist has prepped the tooth.
"I can only support something based on quality," he said. "I have reservations about DHATs, and what I've heard does not sound like a good solution for New Mexico."
Kevin Robertson, executive director of the Kansas Dental Association, said his group wants to create a new level of hygienists who would provide palliative care but would not diagnose or do surgical procedures. "We do not believe it's appropriate training for the types of surgical services they would provide," he told DrBicuspid.com.
Peter Taylor, executive director for the Vermont State Dental Society, said his group has not taken a position on DHATs. "We have not drawn a line in the sand," he told DrBicuspid.com. "This is a broad problem, and I don't think any one answer is going to be the solution." He also recommended increasing state and federal Medicaid funding.
Dental Therapist Project Director Jordan believes that dentists' businesses will be enhanced by therapists' work.
"This is really about improving the ability of dentists to expand their reach," he said. "At the end of the day, it will mean more patients for the dentist because they'll be part of the practice, they can bill for their services, and it gives the dentist more flexibility to see and treat more patients."
What's the solution?
Despite these compelling arguments, there are dentists in the U.S. who support the dental therapist model. Terry Batliner, DDS, who has a private practice in Denver and is the associate director for the Center for Native Oral Health Research, part of the University of Colorado's School of Public Health, believes that properly trained dental therapists can safely do extractions.
"I think you can train people to competently remove mobile primary and permanent teeth and periodontally involved teeth that are loose because they're fairly easy to extract," he told DrBicuspid.com.
Dental therapists receive 3,000 hours of instruction in prepping and restoring teeth, he added -- more than dental schools require. "Dental therapists actually get more hours of training in prepping and restoring teeth than dental students," Dr. Batliner said.
"They've been doing it for several years in Alaska and many other countries, and it's been shown that the quality is no different than if a dentist does it within their scope of practice," he said. "I challenge anyone to identify a study that shows dental therapists anywhere have produced harm."
Critics who contend it would create a secondary system of inferior dental care for the poor should realize that is what we have now, he said.
"We have a two-tiered system now: People who have dental insurance or money can get access to high-quality dental care," Dr. Batliner said. "But the fact is that people who live in rural areas or inner cities who are economically disadvantaged do not have adequate access to care."
Incentives such as loan forgiveness programs aren't enough to keep new dentists in remote or low-income areas, he added. The average dental student graduates with several hundred thousand dollars of debt, he noted.
The Indian Health Service can't fill positions despite offering loan forgiveness and scholarships, Dr. Batliner pointed out. "It's not a long-term solution; dentists go there for a period of time to fulfill their obligation, then they leave," he said.
He attributes the opposition of the dental community to three factors. "I think it's about turf, money, and fear," Dr. Batliner said. "It's clear the old approach doesn't work, so what's their solution?"
Copyright © 2010 DrBicuspid.com