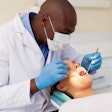
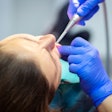
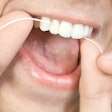
The witnesses called to testify before a U.S. Senate subcommittee February 29 brought stories of unmet dental needs across the country.
And Sen. Bernard Sanders (I-VT), who called the hearing, said he had stories of his own -- some 1,200 of them, gathered from his constituents and other Americans. They were personal accounts, Sanders said, of the struggles that poor, elderly, and working Americans face trying to find and pay for dental care.
"We are in the midst of a dental crisis in America," said Sanders, who chairs the Senate Subcommittee on Primary Health and Aging and released a report to coincide with the hearing. "More than 47 million people live in places where it is difficult to get dental care. We don't have enough providers to serve all of those in need."
The hearing was called to explore the problems with the high cost of care and the lack of access to it, Sanders noted. The witnesses included oral health experts with sobering statistics and providers who said they had found innovative ways of reaching poor and underserved people within their communities.
“We are in the midst of a dental crisis in America.”
— Sen. Bernard Sanders (I-VT)
The lack of access comes at a high cost, not just in human suffering but in tens of millions of misspent state healthcare dollars, said Shelley Gehshan, director of the Pew Children's Dental Campaign. She cited a Pew study released this week that estimated that preventable dental conditions were the primary diagnosis in more than 830,000 emergency room visits in 2009, a 16% increase over 2006.
"Prevention is the most cost-effective way to improve dental health," said Gehshan, who served on the Institute of Medicine's Committee on Oral Health Access to Services last year.
Low-cost treatments, such as dental sealants are still reaching only a fraction of high-risk children in many states. And while water fluoridation has also been shown to reduce decay, she said, "74 million Americans on public water systems lack fluoridated water."
Gehshan called for improvements to the nation's oral health infrastructure, a stronger system of federally qualified health centers to provide preventive and restorative care, and an expanded oral health workforce, including new types of midlevel providers.
New workforce models
One of those providers was witness Christy Jo Fogarty, a dental hygienist and practicing dental therapist. She graduated in June 2011 with a Master of Science degree from the new Oral Health Care Practitioner program at Metropolitan State University in Minnesota.
Comparing her role to that of a nurse practitioner, Fogarty works at a nonprofit clinic under collaborative agreements with several dentists and serves between six and 10 patients a day. She offers referrals, performs triage, and provides a range of restorative procedures, including pulpotomies, stainless-steel crowns, extractions, and fillings. She said she has the satisfaction of providing care to children who might not otherwise get it.
"On one occasion I saw a two-year-old boy who had fallen and hit his front tooth. After a week had gone by without dental care, the tooth had turned dark and was causing him pain," she said. "By the time I saw him, the tooth was traumatized beyond repair. I performed the necessary extraction to relieve the pain and eliminate the infection."
The child's mother told Fogarty she had spent hours searching for dental care but was turned away by a number of offices because of her lack of insurance and the boy's young age.
"She said we were the last call she was going to make before she brought him to the emergency room," Fogarty told the subcommittee. "This would have been a huge expense on the public health system with no conclusive treatment."
Another solution
Vermonter Grant Whitmer, executive director of a Rutland, VT-based federally qualified health center (FQHC), also spoke of filling a critical need. He said his organization started providing dental services in 2007 out of a rented office in an old house using donated equipment.
"Our dental experience was truly a case of 'if you build it, they will come,'" said Whitmer.
The clinic quickly found itself overwhelmed and in need of expansion, with a three-month waiting list of patients, he said. In 2012, the new eight-chair facility expects to provide 12,000 dental visits to almost 4,000 patients, offering free and discounted care worth more than $350,000.
While providing dental care has been a large investment, Whitmer anticipates cost savings in avoided emergency room visits, particularly by adult Medicaid recipients, many of whom were unable to find care because of a shortage of local dentists accepting new Medicaid patients.
Because of their integrated medical home model, FQHCs provide an effective venue for expanding access to dental care in underserved communities, Whitmer said.
School-based clinics
In Louisiana, most of the state's 776,000 Medicaid-eligible children have lacked dental care, according to Gregory Folse, DDS, who told the subcommittee of his experiences establishing school-based clinics to reach them.
While his efforts touched off a towering debate over the rules for mobile dentistry that embroiled the Louisiana State Board of Dentistry, the Louisiana Dental Association, the state Legislature, and the Federal Trade Commission, Dr. Folse eventually prevailed and thousands of schoolchildren in New Orleans, Baton Rouge, and Shreveport are now getting care, he noted.
"On the ground, the truth for me about oral disease and poor access to dental care is clear and undeniable," said Dr. Folse, who also maintains a mobile practice that provides care to 24 nursing homes. "Poor children and aged, blind, and disabled adult Americans suffer needlessly with painful and infected teeth and gums and other unhealthy oral conditions."
He asked the senators to move forward with legislation that would establish a national Medicaid infrastructure for aged, blind, and disabled adults.
Also calling for Congressional attention to adult Medicaid benefits was Burton L. Edelstein, DDS, a professor of dental medicine and health policy at Columbia University and founder and chair of the Children's Dental Health Project, a Washington-based advocacy organization.
"I cannot stress enough that Congress, in its decisions about coverage, has only very recently recognized that dental services are essential to basic, primary health care -- and then, only for children," said Dr. Edelstein. "The record is clear that Congress considers dental care to be an 'optional service' for adults. For adults it's missing in Medicare, largely absent in Medicaid, and unaddressed in health reform."
Dr. Edelstein urged the Senate panel to fully implement the oral health provisions of the federal healthcare reform law known as the Patient Protection and Affordable Care Act as they apply to children.
No witness representing the ADA was called to testify before the subcommittee. But in a statement the organization said it welcomed the hearing "in the hope it would spur lawmakers to address the many barriers to oral health while rejecting the suggestion that there can be a simple fix to the problem. Overall, the nation suffers from lack of understanding about the importance of dental health as part of one's overall health."