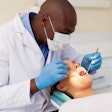
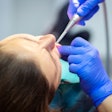
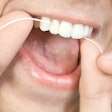
Public health experts who gathered in Washington, DC, on August 17 for a forum on the U.S. oral healthcare crisis clearly agreed on one thing: There is no single solution that will fix the system, which currently leaves tens of millions of Americans without dental care.
A good start might be to begin looking at the oral healthcare delivery as part of the larger healthcare system because many of the challenges are shared, according to David Krol, MD, a pediatrician who helped moderate the forum, entitled "Oral Health: Putting the Teeth into the Health Care System."
"There are racial and ethnic and geographic disparities, challenges with access to care. There are financial challenges and issues of determining and maintaining quality of care. There are workplace controversies, just like with overall health," said Dr. Krol, a program officer for the Robert Wood Johnson Foundation.
The giant healthcare philanthropic organization cosponsored the event with the nonprofit, nonpartisan Alliance for Health Reform, which organizes healthcare briefings and events, including an annual bipartisan healthcare retreat for members of Congress.
“When people turn 65 in this country, we apparently no longer care about their oral health.”
— Lynn Douglas Mouden, DDS, chief
dental officer, CMS
"There is a great opportunity for all makes and models of patients, providers, and policymakers to play a role in improving oral health," Dr. Krol said.
Yet gaps in the system are persistent and formidable. An estimated 100 million Americans currently lack insurance coverage for dental care, a problem that the Patient Protection and Affordable Care Act (PPACA) only partially addresses, program organizers observed. While the healthcare reform act ensures dental benefits for children as part of an "essential health benefits," adults are not guaranteed the same oral healthcare benefits.
In addition, poor children are entitled to dental care under Medicaid, but only a minority of dentists participate in the program. Benefits for poor adults under Medicaid vary from state to state, are often meager, and are vulnerable to cuts during times of fiscal austerity.
"Obviously we are still concerned that in an underserved area a child has dental services until 21 and then we just cut them loose," said panelist Lynn Douglas Mouden, DDS, the chief dental officer for the Centers for Medicare and Medicaid Services (CMS). "That doesn't mean their dental problems or need for dental care has gone away. We are still in a position where it's up to the states to decide whether or not they are going to provide adult dental services under Medicaid. And with competing state priorities, it is still going to be a concern."
Elders on Medicare do not receive coverage for routine care either, Dr. Mouden added.
"When people turn 65 in this country, we apparently no longer care about their oral health," he said. Noting that he, too, was approaching retirement age, he added, "I hope that Medicare will catch up by the time I get there."
More emphasis on prevention needed
Doing a better job of preventing disease in the first place is key to helping future generations, according to Dr. Mouden. "The combination of dental sealants and community water fluoridation can prevent virtually all decay in children," he said.
“It is the wrong care at the wrong place at the wrong time for desperate patients.”
— Julie Stitzel, Pew Center on the
States
Yet there are barriers to meeting those goals. Currently, only an estimated 64% of Americans have access to optimally fluoridated water, according to the Centers for Disease Control and Prevention. In some communities, fluoride opponents have mounted successful campaigns to end the programs.
About 49 million Americans live in rural or poor places with a shortage of dental providers. Many of the children at highest risk lack access to preventive treatments such as sealants that could protect them from disease.
The CMS has set a goal of increasing by 10% the number of Medicaid and SCHIP children receiving a preventive dental service by 2015, Dr. Mouden said. The agency is also working with states to voluntarily develop oral health action plans for identifying and addressing barriers to care.
"We want to know what has succeeded and what might not have been so successful,"Dr. Mouden said.
As it is, increasing numbers of Americans without access to routine care have been turning to emergency rooms for relief of dental pain and infection, said Julie Stitzel, manager of the children's dental campaign at the Pew Center on the States. Her organization estimates that preventable dental conditions were the primary diagnosis in 830,590 visits to emergency rooms in 2009, a 16% increase from 2006. The visits are costly to states and often do not address the patients' needs.
"It is the wrong care at the wrong place at the wrong time for desperate patients," Stitzel said. She spoke in favor of extending care to underserved communities through the use of technically trained dental therapists.
Alternative workforce models
Dental health aide therapists (DHATS) have been working in tribal areas of Alaska for several years. Now another variation of the model is being tested in Minnesota.
Panelist Christy Jo Fogarty, DT, RDH, one of the first certified therapists in the state, compared her role to that of a nurse practitioner. She said she was already an experienced dental hygienist when she underwent a 27-month training program and obtained her new license.
Now, working in collaboration with dentists but trained to a much narrower scope of practice, she provides preventive and restorative care, including stainless steel crowns, pulpotomies, and primary-tooth extractions, to patients in poor and isolated parts of the state.
She recalled getting a return visit from a young boy whose damaged and aching tooth she had extracted. The child ran up to her and gave her a hug.
"You are the lady who took his pain away," the child's mother told Fogarty.
"This is why I do what I do," Fogarty told the Capitol Hill audience.
Though therapists have been widely used in other countries, the model has been strongly opposed by the ADA, a fact that was stressed by panelist Monica Hebl, DDS, vice chair of the ADA's Council on Access. A practicing dentist in Milwaukee, Dr. Hebl said the association does not support the creation of new workforce models that are allowed to perform irreversible procedures.
"With the scarce resources available, we believe a lot more can be done with the current delivery system," she said. "There are 20 new [dental] schools in the pipeline. We should take the current members of the team and use them to their highest capacity."
Dr. Hebl advocated structural improvements in state dental Medicaid programs to make it easier for dentists to treat eligible patients. She also pointed to volunteer initiatives such as the Give Kids A Smile program, which since 2006 has expanded beyond providing a free day of care each year to include a focus upon the establishment of dental homes for children who lack them.
When audience members were given a chance to offer comments and ask questions, Alice Horowitz, PhD, a research associate professor at the University of Maryland School of Public Health, called for wider oral health literacy efforts that emphasize fluoridated water and toothpaste.
Horowitz also expressed impatience with the ongoing debate over workforce models, calling it a fight over "who gets to hold the drill to fill the holes we could have prevented."