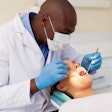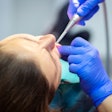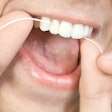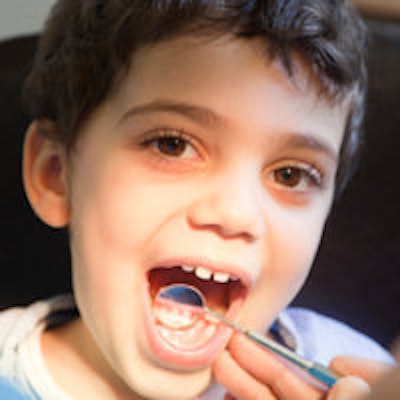
Children enrolled in the Children's Health Insurance Program (CHIP) had higher rates of dental access and more checkups than privately insured children, but fewer in the program actually visited dentists, according to a new federal report released March 30.
The 36-page report concludes that more children are covered by the program, and these children have improved access to healthcare. The report was released by the U.S. Government Accountability Office (GAO) and included data from 10 states.
The CHIP is a joint federal-state program that finances health insurance for more than 8 million children. Since the program's inception in 1997, the percentage of uninsured children nationwide has decreased by half, from 13.9% in 1997 to 6.6% in the first three months of 2014, according to the report.
CHIP covers a full range of health and dental needs of millions of children and is critical for their health and future well-being, according to Meg Booth, MPH, director of policy for the Children's Dental Health Project (CDHP). Booth said this program is essential to millions of working families as it provides affordable comprehensive health coverage to millions of children and 370,000 pregnant women from working families who earn too much to qualify for Medicaid but cannot afford private coverage.
 Colin Reusch, senior policy analyst, Children's Dental Health Project. Image courtesy of CDHP.
Colin Reusch, senior policy analyst, Children's Dental Health Project. Image courtesy of CDHP.Colin Reusch, a senior policy analyst with the CDHP, is an expert on the Patient Protection and Affordable Care Act's pediatric dental benefit. CHIP not only provides coverage for enrolled children, it also keeps costs down, he said.
"While more needs to be done to ensure that children get the care they need, it's important to keep in mind the fact that unmet dental need would be significantly higher without CHIP," Reusch told DrBicuspid.com.
He explained the importance of continued funding for the CHIP program.
"The GAO report notes that children enrolled in CHIP have greater access to dental coverage than children with private insurance," Reusch said. "And even when privately insured children have comprehensive dental coverage, the out-of-pocket costs are much higher than what families encounter in CHIP."
Children in the program were more than a third more likely to have a usual source of dental care and were almost 40% more likely to have had a dental checkup in the past year compared with uninsured children, the report said.
Enrollees also had higher rates of dental access and utilization of certain services. More than 90% of children in the program had access to dental coverage in 2012, compared with 77% of privately insured children. In terms of utilization, 84% of CHIP enrollees had a dental checkup or cleaning in the previous 12 months, compared with 79% of privately insured children.
“While more needs to be done to ensure that children get the care they need, it's important to keep in mind that unmet dental need would be significantly higher without CHIP.”
However, a lower proportion of children in the program visited dentists (42.4% compared with 50.9%) and orthodontists (4.9% compared with 11.2%) within the past 12 months than did those who were privately insured, the report noted.
Specifically, many children in the program did not receive recommended preventive care or reported an unmet healthcare need. For example, 1 in 4 CHIP enrollees had an unmet healthcare need, with the highest unmet need being for dental care.
Less than half (46%) of CHIP enrollees received at least one preventive dental service, and only a quarter of the children received at least one dental treatment in 2013, the report found.
The report concluded that families could face higher dental costs in states where dental coverage through state-run insurance exchanges is optional and offered as a standalone dental plan, as opposed to CHIP plans in which dental benefits are included.
U.S. Senate action
The U.S. House of Representatives overwhelmingly passed a bill on March 26 to continue funding the CHIP program, but the Senate is in recess through April 12. The bill will likely be put to a vote when the Senators return.
The CHIP program is currently set to expire on September 30. If passed by the Senate and signed by President Barack Obama, the bill, HR 2, will extend CHIP coverage for another two years.
Regarding access to care, several states raised concerns about negative implications for children's coverage if CHIP funding is not reauthorized, including concerns that their states would lose gains made in covering children and that children would also lose access to providers and dental care, the report concluded.
Reusch stressed how the program improves the overall health of children, noting widespread support for funding the program for four more years.
"This is why 20 dental organizations recently signed a letter urging Congress to extend federal funding for CHIP," Reusch said.